Summary: A degloved face is a serious medical emergency where the skin and soft tissue are forcibly torn away from the underlying facial muscles and bones, cutting off blood supply. It is most commonly caused by high-speed road accidents, industrial machinery, and violent assaults. Treatment requires immediate emergency surgery, wound care, and often multiple reconstructive procedures. Recovery is long, involving physical rehabilitation and psychological support. Prevention centres on wearing appropriate protective gear in high-risk environments.
A degloved face is one of the most severe traumatic injuries a person can sustain — and one of the least talked about in everyday health conversations. Yet understanding what it is, how it happens, and what treatment looks like can make a critical difference in how quickly someone receives life-saving care.
Whether you are a healthcare professional, a concerned family member, or someone researching facial trauma for safety awareness, this guide covers everything you need to know — clearly, honestly, and without unnecessary fear-mongering.
Table of Contents
What Is a Degloved Face?
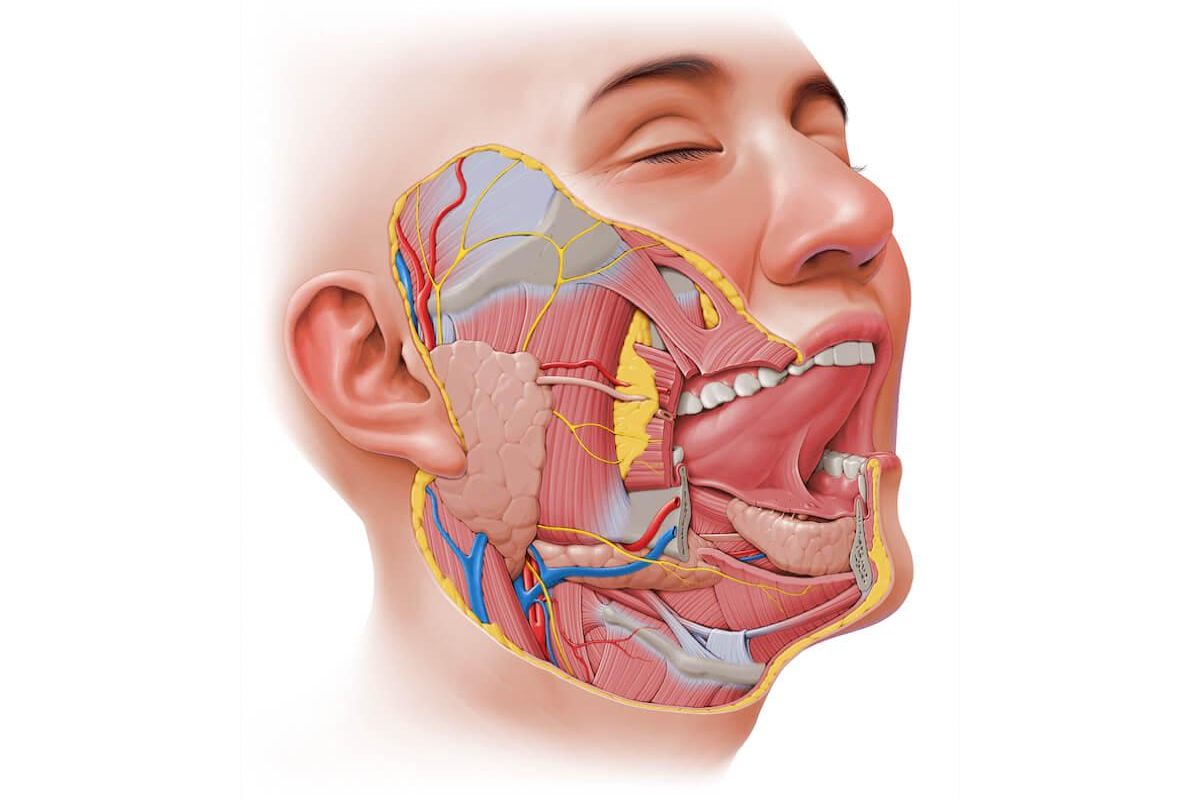
A degloved face — also called a facial avulsion injury — occurs when the skin and soft tissue layers of the face are violently torn away from the underlying structures: the muscles, connective tissue, and in severe cases, the facial bones themselves.
The name comes from the analogy of removing a glove: the skin peels back from the face the way a glove strips off a hand, exposing the raw anatomical structures beneath.
According to WebMD’s clinical overview of degloving injuries, these injuries cause the top layers of skin to lose their blood supply even when they remain partially attached as a flap — which is why immediate emergency treatment is non-negotiable.
Facial degloving injuries can range from partial (affecting a small area such as the nose or eyelid) to complete (involving large sections of the face including the forehead, cheeks, lips, and scalp).
How Common Are Degloved Face Injuries?
Degloved face injuries are considered rare but life-threatening. The majority of cases are reported in:
- Road traffic accident survivors (especially motorcyclists and unrestrained vehicle occupants)
- Industrial workers exposed to heavy or rotating machinery
- Victims of violent assault
- Patients involved in agricultural accidents
Hemifacial degloving — affecting one full side of the face — is documented in peer-reviewed literature as extremely rare. A published case study in the NIH’s PubMed Central on face avulsion and degloving notes that most patients with severe hemifacial degloving do not survive long enough to reach hospital care due to associated head and vascular injuries — underscoring how critical the minutes immediately after injury are.
Types of Degloved Face Injuries
Degloving injuries are classified into two primary categories:
1. Open (External) Degloving
This is the more immediately visible and severe form. In open degloving:
- The skin and tissue are physically ripped away, leaving muscles, bones, tendons, or blood vessels exposed
- The skin may be completely detached or still hanging as a partial flap
- Bleeding is severe and infection risk is immediate
- On the face, open degloving most commonly affects the nose, forehead, cheeks, eyelids, and scalp
2. Closed (Internal) Degloving
Closed degloving is harder to diagnose because the external skin surface may appear relatively intact:
- Internally, the skin and fat layer are separated from the deeper muscle and connective tissue
- A pocket forms under the skin, filling with blood and lymphatic fluid
- This is clinically known as a Morel-Lavallée lesion
- On the face, closed degloving is significantly less common than open injuries
Causes of a Degloved Face
The following are the primary mechanisms that produce facial degloving injuries:
Road Traffic Accidents High-speed collisions — particularly motorcycle crashes and accidents where occupants are unrestrained — generate the shearing forces necessary to tear facial tissue from bone. The face strikes surfaces (windscreen, road, dashboard) at extreme velocity.
Industrial and Agricultural Machinery Equipment involving rotating parts, conveyor belts, or heavy rollers poses a documented risk. Hair or clothing caught in machinery can produce avulsion injuries affecting the face and scalp.
Violent Assault Attacks using bladed weapons, blunt objects, or bites (including animal attacks) can cause localised or extensive degloving of specific facial areas including the nose, lips, and periorbital (eye socket) region.
Falls from Height Significant falls — especially onto hard or rough surfaces — can generate enough trauma force to cause partial facial degloving, often combined with other maxillofacial fractures.
Blast Injuries Explosive force in industrial or conflict settings can produce complex, multi-site facial degloving.
Signs and Symptoms to Recognise
Identifying a degloved face injury quickly is essential to survival and functional recovery.
Visible signs include:
- Skin and tissue torn back or hanging from the face
- Exposed muscle, bone, or blood vessels
- Severe, active bleeding
- Swelling and bruising extending beyond the wound site
- Pale, waxy skin at the injury margin (indicating blood supply loss)
Less obvious but critical signs:
- Intense, disproportionate pain
- Numbness in facial areas (nerve involvement)
- Difficulty opening the jaw or moving facial muscles
- Signs of shock: rapid pulse, pale skin, confusion, rapid breathing
It is important to note that a degloved face is also a deeply traumatic psychological experience. Many survivors describe the emotional impact as equal to or greater than the physical injury — something that must be acknowledged in any comprehensive treatment plan.
Emergency First Response: What to Do
If you witness or experience a suspected degloved face injury, the following steps are critical before professional medical help arrives:
- Call emergency services immediately — this is not an injury manageable at home or with first aid alone
- Do not attempt to reattach or reposition tissue — this risks further vascular damage and contamination
- Control bleeding with gentle, clean pressure — avoid direct pressure on exposed tissue or bone
- Keep the person still and calm — movement increases blood loss and shock risk
- If skin flaps are detached, wrap them in a clean, damp cloth and bring them to the hospital — surgeons may be able to use them in reconstruction
- Monitor for signs of shock and maintain airway patency if the person is conscious
Medical Diagnosis
On arrival at emergency care, the medical team will:
- Conduct a rapid trauma assessment to prioritise life-threatening injuries
- Examine the wound under anaesthesia to determine the full extent of tissue and vascular damage
- Order imaging (CT scan, X-ray) to identify associated fractures and structural damage
- Assess skin viability — determining which tissue can be saved and which cannot
As noted by MedicineNet’s clinical guide on degloved face injuries, visually assessing degloved skin alone is unreliable — surgeons use multiple clinical criteria including tissue bleeding response, colour, temperature, and pressure reaction to determine viability.
Treatment of a Degloved Face
Treatment of facial degloving is complex, staged, and requires a multidisciplinary surgical team including plastic surgeons, maxillofacial surgeons, and trauma specialists.
Stage 1: Emergency Stabilisation
- Airway management and breathing support
- Control of haemorrhage (blood loss)
- Prevention of shock and infection
- IV fluid resuscitation
Stage 2: Surgical Intervention
- The wound is thoroughly cleaned (irrigated with saline) and debrided — dead or contaminated tissue is removed
- The degloved skin flap, where viable, is repositioned and sutured back to its anatomical position
- Facial fractures are repaired simultaneously where possible
- If the original skin cannot be saved, skin grafting is performed using tissue from another part of the body (thigh, back)
- In major reconstructions, local or free flaps (tissue transferred with its own blood supply) may be used to rebuild nasal, eyelid, cheek, or lip structures
Stage 3: Post-Operative Wound Care
- Regular dressing changes to prevent infection
- Monitoring of graft or flap survival
- Antibiotic therapy as indicated
Stage 4: Reconstructive Surgery (Staged)
Most facial degloving cases require multiple surgical procedures over months or years to achieve functional and aesthetic outcomes. This may include:
- Scar revision surgery
- Nasal or eyelid reconstruction
- Nerve repair procedures
- Dental and jaw reconstruction if fractures were involved
Recovery: What to Expect
Recovery from a degloved face injury is a prolonged, demanding process. There is no single timeline — severity, age, overall health, and the quality of initial treatment all influence outcomes.
Physical recovery considerations:
- Initial hospitalisation typically lasts days to weeks depending on injury severity
- Graft and flap healing requires careful monitoring for 2–4 weeks post-surgery
- Scar tissue maturation takes 12–24 months — final cosmetic results are not assessable before this point
- Physical therapy may be required to restore facial movement and reduce scar contracture
Long-term effects that may persist:
- Visible scarring
- Reduced or altered sensation in facial areas
- Impaired facial movement (if nerve damage occurred)
- Vision complications if periorbital structures were involved
- Chronic pain
Psychological recovery: This is a dimension that receives insufficient attention in many clinical overviews. Survivors of degloved face injuries commonly experience:
- Post-traumatic stress disorder (PTSD)
- Depression and anxiety related to altered appearance
- Social withdrawal and reduced quality of life
- Body dysmorphia concerns during the reconstruction period
Psychological support — including trauma-focused therapy, counselling, and peer support groups — is an essential, not optional, component of full recovery.
Common Mistakes in Managing Degloved Face Injuries
Delaying emergency care Even if the person seems stable, internal vascular damage and blood loss can deteriorate rapidly. Every minute between injury and surgery affects tissue viability and survival rates.
Attempting home management No degree of first aid substitutes for emergency surgical intervention. Attempting to clean or dress a degloved wound improperly increases infection risk and can damage viable tissue.
Discarding detached skin Detached skin flaps should always be preserved, wrapped in a moist clean cloth, and transported with the patient. Surgeons can sometimes use the original tissue in reconstruction.
Neglecting psychological care Physical healing without psychological support leads to poor quality-of-life outcomes. Mental health care should begin as early as the acute treatment phase and continue throughout the recovery journey.
Prevention: Reducing Your Risk
While no prevention strategy eliminates all risk, the following significantly reduce the likelihood of facial degloving injuries:
| Setting | Preventive Measure |
|---|---|
| Road travel | Wear a full-face helmet (motorcyclists); use seatbelts |
| Industrial workplace | Follow machinery safety protocols; use facial shields |
| Agricultural environments | Ensure hair and clothing are secured near rotating equipment |
| Contact sports | Wear appropriate facial guards and helmets |
| Violent conflict situations | Situational awareness and personal safety planning |
| Vehicle occupants | Ensure airbags are functional; avoid distracted driving |
Myths vs Facts: Degloved Face
| Myth | Fact |
|---|---|
| It only happens in extreme accidents | Even moderate-impact collisions can cause degloving in vulnerable facial areas |
| Detached skin cannot be reused | Surgeons can and do use viable degloved tissue in reconstruction |
| Full recovery is always possible | Outcomes vary; permanent scarring and functional changes are common |
| It only affects adults | Children involved in road or machinery accidents are equally vulnerable |
| Recovery takes a few weeks | Full physical and psychological recovery often takes 1–3 years |
FAQs: Degloved Face
Q: What is a degloved face? A: A degloved face is a severe traumatic injury where the skin and soft tissue are torn away from the underlying facial muscles, connective tissue, or bones, cutting off blood supply to the affected area.
Q: Is a degloved face always fatal? A: Not always, but it is life-threatening. Survival depends on the speed of emergency response, extent of injury, and presence of associated head or vascular trauma.
Q: Can a degloved face be reconstructed? A: Yes, through staged reconstructive surgery involving skin grafts, tissue flaps, and multiple surgical procedures over months or years. Outcomes vary significantly by injury severity.
Q: What is the most common cause of a degloved face? A: High-speed road traffic accidents are the leading cause, particularly motorcycle crashes and collisions involving unrestrained occupants.
Q: How long does recovery from a degloved face take? A: Physical recovery from initial surgery takes weeks to months. Full scar maturation and final cosmetic outcomes may not be apparent for 12–24 months. Psychological recovery may take longer.
Q: Is a degloved face the same as a facial fracture? A: No. Facial fractures involve broken bone; degloving involves the tearing of skin and soft tissue. Both can occur simultaneously in severe trauma.
Q: What should you do if you witness a degloved face injury? A: Call emergency services immediately. Do not attempt to reattach tissue. Apply gentle pressure to control bleeding. Preserve any detached skin in a clean, moist cloth. Keep the person calm and still.
Final Conclusion
A degloved face is among the most severe and complex injuries in trauma medicine — one that demands immediate emergency response, expert surgical care, and sustained physical and psychological rehabilitation. Understanding its causes, recognising its signs, and knowing the correct emergency steps can genuinely save a life or preserve critical tissue that determines a person’s long-term recovery outcomes.
Prevention remains the most powerful tool we have: wearing full-face helmets, following workplace safety protocols, and practising responsible road behaviour are simple, accessible choices that dramatically reduce the risk of experiencing a degloved face injury in the first place.
If you found this article helpful, explore more health and safety guides on HealthCaresBlog.com — because informed readers make safer decisions every single day.