Summary Charlotte Gastroenterology & Hepatology (CGH) is a group of 6 patient-centered, independent, physician-owned GI specialty practices in Charlotte, NC. They have been in practice for over 40 years, which includes a total of 23 gastroenterologists who are all boardcertified. They offer the full scope of services in Gastroenterology and Hepatology for a wide range of diseases and disorders. Here is a detailed summary of what CGH offers, who is a candidate for care and what to expect prior to your first visit.
If you are experiencing persistent, rather than occasional, stomach difficulty or your doctor has urged you to come in for a colonoscopy or some unknown procedure, or to see if you have problems with your liver you may have heard of Charlotte Gastroenterology & Hepatology (CGH). You‘re wondering who they are and how they might help you.
This page can genuinely provide you with an honest, medically informed answer to all of those questions.
Table of Contents
What Is Charlotte Gastroenterology & Hepatology?
Located in Charlotte, N.C., Charlotte Gastroenterology & Hepatology is an independent specialty practice devoted solely to the digestion system and liver. Opposed to a hospital-employed GI group, CGH is owned by physicians: your treatment decisions are made by the doctors that take care of you… not a corporate bank of administrators.
This established practice has cared for patients in the greater Charlotte region for over four decades and is comprised of 22 board certified and highly trained physicians with specialized expertise in advanced biliary endoscopy, liver disease and liver transplant assessment.
CGH has a patient base of over 125,000 and operates across the Charlotte region, which has a population of over 2.5 million people. Charlottegastro They have six clinic locations — including Randolph Road (their main hub), Ballantyne, Huntersville, Mooresville, Matthews, and SouthPark — and conduct endoscopic procedures at several of those offices.
Their ad slogan, “Trust Your Gut to the Experts,” sums it up, what differentiates a devoted GI practice from a primary care office or urgent care: you are seen by a doctor who specializes in and cares solely for the gastrointestinal system.
Who Charlotte Gastroenterology & Hepatology Is Best For
Gastroenterology is not a one-condition specialty. CGH is relevant to a wide range of patients, from someone needing their first routine colonoscopy to someone managing a complex chronic liver disease.
You should consider booking an appointment if you:
- Are 45 or older and have never had a colorectal cancer screening
- Have persistent symptoms — heartburn, bloating, abdominal pain, irregular bowel habits, or rectal bleeding — lasting more than a few weeks
- Have been diagnosed with or suspect Crohn’s disease, ulcerative colitis, GERD, IBS, or celiac disease
- Have a family history of colon cancer, inflammatory bowel disease, or liver conditions
- Have abnormal liver enzymes, yellowing skin (jaundice), or unexplained fatigue alongside digestive symptoms
- Have been referred for a specific procedure like an ERCP, endoscopic ultrasound, or capsule endoscopy
- Are managing chronic hepatitis B, hepatitis C, fatty liver disease (NASH/NAFLD), or cirrhosis
You may be better served at a large academic medical centre if:
- You require complex liver transplant surgery (CGH evaluates for transplant but surgery is performed at a transplant centre)
- You have rare paediatric GI conditions (CGH focuses on adult gastroenterology)
- You need multidisciplinary oncology integration for advanced GI cancer treatment
Their ad slogan, “Trust Your Gut to the Experts,” sums it up, what differentiates a devoted GI practice from a primary care office or urgent care: you are seen by a doctor who specializes in and cares solely for the gastrointestinal system.ancreatic disorders.
On the liver and hepatology side, they manage viral hepatitis (B and C), alcohol-related liver disease, autoimmune liver conditions, fatty liver disease, cirrhosis, and provide evaluation and co-management for liver transplant candidates.
Core Procedures and Services at CGH
Colonoscopy and Colorectal Cancer Screening
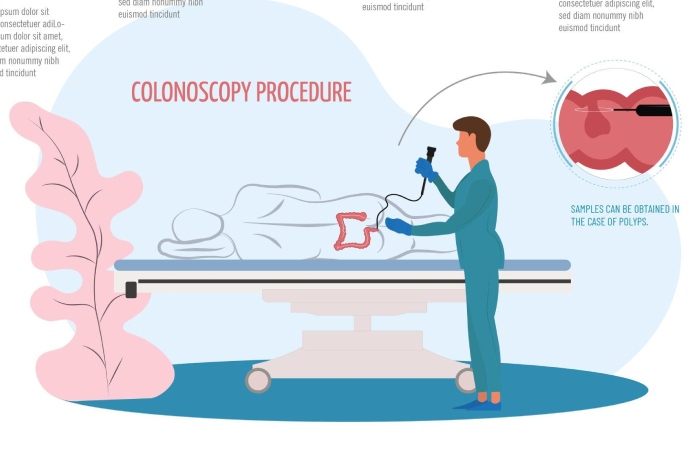 Colonoscopy is the most commonly ordered procedure at any gastroenterology practice and for good reason. The US Preventive Services Task Force has upped the age to set an initial screening for colorectal cancer among adults from 50 to 45. CDC Screening is recommended until age 75 up from the previous age of 50 as colorectal cancer cases increase among young adults.
Colonoscopy is the most commonly ordered procedure at any gastroenterology practice and for good reason. The US Preventive Services Task Force has upped the age to set an initial screening for colorectal cancer among adults from 50 to 45. CDC Screening is recommended until age 75 up from the previous age of 50 as colorectal cancer cases increase among young adults.
The American College of Gastroenterology recommends screening for colorectal cancer in asymptomatic patients between the ages of 45-75 in order to prevent precancerous polyps, reduce the incidence of colorectal cancer, and prevent death from colorectal cancer.
Colonoscopy at CGH is an outpatient procedure which screens for colorectal abnormalities such as Cancer or pre-cancerous diseases. This test is performed by a doctor who inserts a tube (the colonoscope) through your anus and takes a video of the inside of your colon; the image of the lining of the colon is displayed on a computer screen so abnormalities can be seen.
If your risk for colon cancer is higher than average conditions such as family history, inflammatory bowel disease, or previous polyps your gastroenterologist may advise that you start colonoscopy at an age earlier than 45, or repeat colonoscopy more often than 10 years.
Open Access Screening Colonoscopy is available at CGH for appropriate candidates to be scheduled without a prior visit, thus decreasing the wait for routine screening.
Upper Endoscopy (EGD)
An upper endoscopy or EGD (esophagogastroduodenoscopy) is a thin, flexible tube with a camera at the end. It allows the doctor to view the inside of the esophagus, stomach, and first part of the small intestine. An EGD helps doctors look into problems of long-standing heartburn, trouble swallowing, unexplained nausea, ulcers, and suspected Barrett‘s esophagus.
Performed under light sedation, this procedure takes between 15–30 minutes. The patient usually recovers after only a few hours.
Endoscopic Ultrasound (EUS)
EUS or endoscopic ultrasound is a less invasive way to view the interior lining and walls of the upper and lower gastrointestinal tract (stomach, intestines and colon). Using sound waves, incredibly detailed images of the upper and lower GI tract are produced and this information is used for finding the cause of abdominal pain or for identifying, diagnosing or staging certain types of cancer. In addition, it provides important information regarding the pancreas, gall bladder and liver.
EUS may be integral if a lesion suggesting or within the pancreas has been visualized on a CT scan or MRI and tissue acquisition for biopsyin order to establish a diagnosis is necessary. CGH hasphysicians withsubspecialty training in EUSwhich is not available at many other GI practices.
ERCP (Endoscopic Retrograde Cholangiopancreatography)
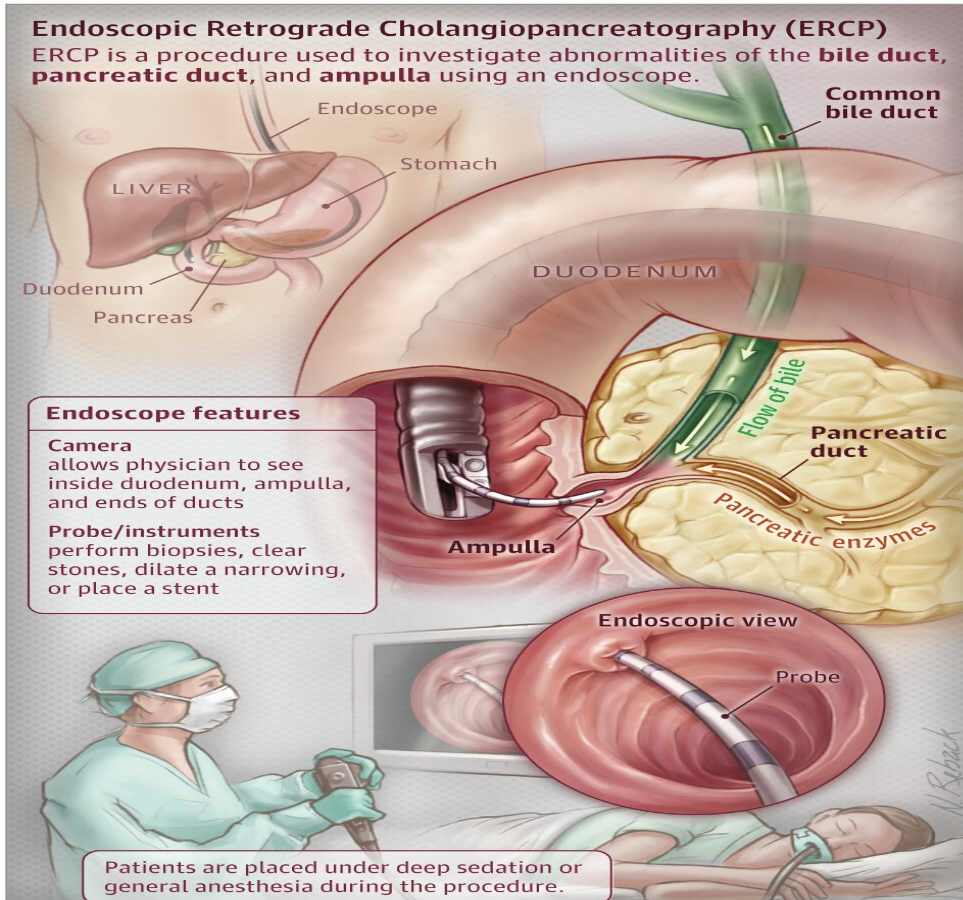
ERCP (Endoscopic retrograde cholangiopancreatography )ERCP is used to investigate the ducts of the gall bladder, pancreas and liver. It is a technique where x–ray and an endoscope are used to view the inside of the stomach, duodenum and the ducts of the biliary tree and pancrease. ERCP can be used to identify the cause of jaundice, upper abdominal pain or unexplained weight loss.
ERCP is diagnostic AND therapeutic, for example the stones in the bile duct can be identified and removed by ERCP, narrowings to the bile duct aka stricutres can be treated and blocked areas can be drained. This is a complex endoscopic procedure so sub specialist training is needed and it is not provided by GPs. CGH employs specific doctors for interventional endoscopy including ERCP.
Capsule Endoscopy
Capsule endoscopy enables doctors to look at the lining of the small bowel (a section of GI tract that can not be seen with an ordinary upper GI endoscopy or colonoscopy). Charlottegastro The patient swallows a small, vitamin-sized capsule that houses a tiny wireless camera. The capsule makes its way through the digestive system over a period of hours and cameras take thousands of pictures which are transmitted to a recording device worn in a belt. Useful for finding the cause of unexplained GI bleeding or suspected Crohn s disease of the small bowel.
Radiofrequency Ablation (RFA) for Barrett’s Esophagus
Radiofrequency ablation is a technique used to treat Barrett‘s oesophagus using radiofrequency waves. It destroys abnormal precancerous and cancerous cells within the Barrett‘s tissue. Barrett‘s oesophagus is a condition where the lining of the oesophagus is changed as a result of long-term reflux. This increases the risk of developing cancer. It is an effective technique in the treatment of Barrett‘s oesophagus.
Breath Testing
A breath test can be used as a non-invasive, pain free, method of diagnosing some gastrointestinal conditions. Now available at Charlottegastro CGH are a number of breath tests for H. pylori (a bacteria which causes gastric ulcers), small intestinal bacterial overgrowth (SIBO), lactose intolerance and fructose malabsorption. These tests are all performed quickly, are non-sedating and can be very useful in directing treatment without the need for Endoscopy.
Fecal Microbiota Transplant (FMT)
Recently being used in practice is FMT, where stool from a healthy tested stool donor is transplanted into the recipient‘s gut to provide the necessary microbiota. It is mainly used in treatment of recurrent C. diff. infection, which if appropriate treatment fails, can be resistant to antibiotics. The use of this in CGH demonstrates drive to practice using evidence based measures.
Infusion Therapy
For the convenience of our patients, our practice has a four-chair infusion center located at our practice on Randolph Road. Charlottegastro Patients with inflammatory bowel disease Crohn‘s disease and ulcerative colitis can receive therapy in our gastroenterology practice with biologic IV infusions including infliximab or vedolizumab rather than having to go to a separate infusion center.
Liver and Hepatology Care at CGH
Hepatology — the subspecialty focused on liver, gallbladder, biliary tract, and pancreas diseases — is one of CGH’s specific areas of deep expertise. Managing liver conditions requires long-term, specialist-led follow-up because many liver diseases progress silently before symptoms appear.
CGH manages hepatitis B and C, NASH (nonalcoholic steatohepatitis, increasingly called MASLD), autoimmune hepatitis, primary biliary cholangitis (PBC), primary sclerosing cholangitis (PSC), and cirrhosis. For patients whose liver disease progresses to end-stage liver failure, CGH provides evaluation and co-management for liver transplant referral, coordinating with transplant surgical centres.
What most patients don’t know: The liver is the only major organ that can regenerate, but that regenerative capacity is significantly diminished once cirrhosis develops. Early diagnosis and management of conditions like NASH or hepatitis — even when the patient feels well — is critical to preventing irreversible damage. This is why a referral to hepatology at the right time matters.
Clinical Research: A Differentiator Worth Knowing
Charlotte Gastroenterology & Hepatology is committed to providing patients with every resource available, including research studies, for the treatment of gastrointestinal and liver disease. For over two decades, CGH has participated in numerous national research studies, including Phase II, III, and IV trials. They are currently enrolling patients in studies covering colon cancer screenings, ulcerative colitis, Crohn’s disease, NASH, and celiac disease.
This is clinically meaningful for patients. Participation in clinical trials can provide access to cutting-edge therapies before they receive full regulatory approval — at no additional cost in many cases. It also means CGH physicians are embedded in the latest research, influencing how they approach treatment for all their patients, not just those enrolled in trials.
What Competitors Miss: The Nuances You Should Know
1. Independent practice matters more than it seems. CGH is physician-owned and independent — not part of a large hospital network. This can affect referral patterns, wait times for procedures, and how quickly decisions are made. For patients who want direct, specialist-led continuity of care, this is a meaningful advantage.
2. Not all GI practices offer the same procedural depth. ERCP, endoscopic ultrasound, capsule endoscopy, RFA, and FMT are advanced services. Many GI practices refer patients elsewhere for these. CGH’s ability to perform these under one roof means fewer referrals, fewer delays, and more coherent care.
3. Colon cancer screening guidelines have changed — and many patients don’t know it. If you turned 45 in the last few years and have not had a colonoscopy, you are overdue. The screening age was lowered from 50 to 45 in recent guidelines precisely because of rising colorectal cancer rates in adults under 50. This is not optional prevention — it is the current evidence-based standard.
4. Fatty liver disease is now the leading cause of liver disease globally — and most patients have no symptoms until it is advanced. NASH/MASLD (metabolic-associated steatotic liver disease) is rapidly increasing alongside rising rates of obesity and type 2 diabetes. A routine blood test showing elevated liver enzymes is often the first — and only — signal. If your GP has flagged abnormal liver function tests, a hepatology consultation at CGH is the appropriate next step, not watchful waiting.
Common Myths About Gastroenterology and Digestive Health
Myth symptom prompted colonoscopy: Fact most colon cancers are asymptomatic in the early, reversible stages. 45, or earlier if you have risk factors, is screening colonoscopy to prevent the hours of feeling perfeclty fine by removing polyps.
Myth: Digestive symptoms such as bloating, wind, altered bowel habits are normal Fact: Chronic digestive symptoms have identifiable, treatable causes. Chronic conditions such as irritable bowel syndrome, small intestinal bacterial overgrowth, coeliac disease, inflammatory bowel disease, gastroesophageal reflux disease can all be diagnosed and treated. Normalising the symptoms delays appropriate treatment.
Myth: Fatty liver disease is a condition for those drinking heavily. Fact: NASH – fatty liver disease associated with the disease metabolic syndrome is thought to now be present in an estimated 25% of adults worldwide and has no association with alcohol consumption. This type of fatty liver is now thought to be caused by the diet, insulin resistance and genetic predisposition.
Myth: Upper endoscopy and colonoscopy are invasive surgical procedures which involve a long hospital stay. Fact: Upper endoscopy and colonoscopy are outpatient procedures carried out under sedation. The majority of patients go home within two hours and resume their normal lives the next day.
Quick Reference: CGH Procedures at a Glance
| Procedure | What It Examines | Primary Uses | Recovery Time |
|---|---|---|---|
| Colonoscopy | Large intestine & rectum | Cancer screening, polyp removal, IBD | 1–2 hours post-procedure |
| Upper Endoscopy (EGD) | Esophagus, stomach, upper small intestine | GERD, ulcers, Barrett’s | 1–2 hours post-procedure |
| Capsule Endoscopy | Small intestine | GI bleeding, Crohn’s | Same day, no sedation |
| EUS | GI walls + nearby organs | Cancer staging, pancreas evaluation | 1–2 hours post-procedure |
| ERCP | Bile ducts, pancreatic duct | Gallstones, duct blockages | 2–4 hours; may require monitoring |
| Breath Testing | Bacterial/enzyme activity | H. pylori, SIBO, lactose intolerance | No recovery needed |
| RFA | Esophageal lining | Barrett’s esophagus treatment | 1–2 hours post-procedure |
| FMT | Gut microbiome | Recurrent C. diff infection | Same day |
What to Do Before Your First Appointment at CGH
- Gather all prior GI-related records. This includes previous endoscopy reports, imaging (CT scans, ultrasounds, MRIs), and lab results — especially liver function tests, complete blood counts, and metabolic panels.
- Write down your symptoms. Be specific about onset, frequency, severity, and what makes them better or worse. Include any blood in stool, unintentional weight loss, or night sweats — these are red flags that will fast-track your evaluation.
- Know your family history. First-degree relatives with colorectal cancer, polyps, IBD, or hereditary syndromes like Lynch syndrome are clinically relevant and will affect your screening schedule.
- Bring a full medication list. Include prescription drugs, OTC medications, supplements, and herbs. Some medications directly affect GI function and liver enzymes.
- If you are being referred for a colonoscopy, ask about prep requirements in advance. Colonoscopy preparation (clearing the bowel) begins the day before the procedure and requires dietary changes and a prescribed laxative preparation. Understanding this upfront reduces anxiety and ensures a clean prep — which directly affects the quality of the examination.
- Use MyChart. Charlotte Gastroenterology & Hepatology offers patient portal access through MyChart, allowing enhanced communication with providers and the ability to communicate with their office at times most convenient to patients.
FAQs
What does Charlotte Gastroenterology & Hepatology do?
CGH specializes in a comprehensive, comprehensive care for all diseases of the adult digestive system and liver. Their areas of depth of knowledge include: advanced biliary endoscopy (ERCP), treatment of liver disease, including transplant evaluation, colonoscopy and screening for colon cancer, inflammatory bowel disease and conducting active clinical trials research.
What age should I have my first colonoscopy?
Current guidelines from the American College of Gastroenterology and the US Preventive Services Task Force suggest screening all average risk adults for colorectal cancer beginning at age 45. You may have to begin at a younger age if your mother or father, sister, or brother has colon cancer or polyps, or you suffer from inflammatory bowel disease. Consult your gastroenterologist.
What is hepatology and if I need it?
Hepatology is the area of gastroenterology subspecialized in the liver, biliary system and pancreas. You may be referred to a hepatologist if you has hepatitis B or C, fatty liverNASH/MASLD, cirrhosis, autoimmune liver disease or abnormal liver function tests which cannot be explained by your GP.
What is ERCP and why is it done?
ERCP (endoscopic retrograde cholangiopancreatography) is a more complex endoscopic technique that looks at and treats in the bile and pancreatic ducts. It can be used to remove bile duct stones, investigate strictures, and unexplained jaundice or pancreatitis. It requires specialised training, and is not currently routinely offered at all GI practices.
Will The CGH accepting insurance?
CGH takes most major insurance plans. Call your location directly to verify your insurance is accepted before your appointment. Colonoscopy for preventive screening is covered with no co-pay for most insured adults under the Affordable Care Act of 2010, but there may be charges if a polyp is found and taken out (changes a diagnostic billing code to a preventive code a known issue worth inquiring about.).
How do I get results and speak with my provider?
CGH has partnered with the MyChart patient portal to access test results, schedule your appointments and message with your care team.
Final Conclusion
In addition to the broad service offerings noted above, if you are presenting for screening at age 45, or are known to have a chronic disorder such as Crohn‘s disease or hepatitis C, or are seeking a more advanced diagnosis such as ERCP or liver workup, there are few general Gastroenterology practices that offer the depth of specialist experience, the spectrum of procedures performed, and the clinical research arm of service that we can.
What sets them apart is not just their 40+ year history or their 23 board certified physicians, but the confluence of independent physician owned practices, subspecialty procedural capability, participation in active clinical trials and six easy to access practice locations across the Charlotte area.
If you have had symptoms for some time, your GP has indicated an out-of-normal test result, or you‘ve hit the age where you can‘t opt out of preventive screening anymore, Charlotte Gastroenterology & Hepatology is an established first step toward the answers and treatment you need. Schedule an appointment online or through their MyChart portal and bring along your records and symptom history you are in the experts’ care.
